 
Positron emission tomography (PET) has a relatively lower sensitivity (80.3%) and specificity (92.8%) in the evaluation of metastatic nodes, but the sensitivity (91.8%) and specificity (98.9%) are higher when PET/CT is used. On high resolution MRI, the sensitivity and specificity in assessing metastatic nodes are 86% and 94% respectively, whereas those in evaluating lymphomas are 85% and 95% respectively. On contrast-enhanced CT, the reported sensitivity and specificity in the evaluation of metastatic cervical lymph nodes are 90.2% and 93.9% respectively. 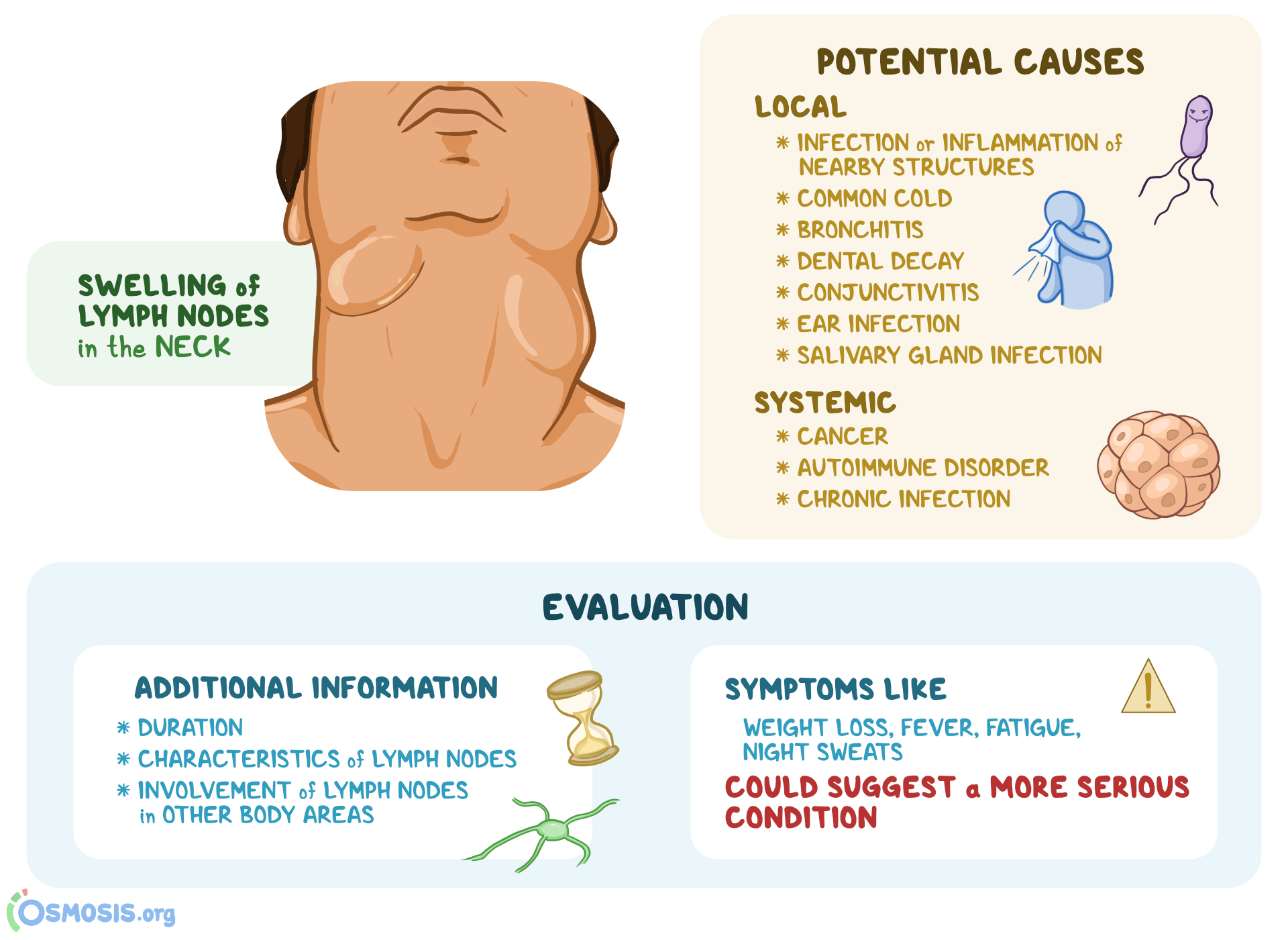
In addition, MRI may not identify intranodal calcification which is a useful feature in predicting metastatic nodes from papillary carcinoma of the thyroid,. Although computed tomography (CT) and magnetic resonance imaging (MRI) are also used to evaluate cervical lymph nodes, the nature and internal architecture of small lymph nodes (<5 mm) may not be readily assessed. When combined with guided fine needle aspiration cytology (FNAC), the specificity of ultrasound is as high as 93%. It is particularly sensitive compared to clinical examination (96.8% and 73.3% respectively) in patients with previous head and neck cancer with post-radiation neck fibrosis. The role of ultrasound in the assessment of cervical lymphadenopathy is well established. As the treatment options differ, accurate identification of the nature of the diseases is essential. Clinically, lymphomatous cervical lymph nodes are difficult to differentiate from other causes of lymphadenopathy including metastatic nodes. īesides metastases, lymphoma is also a common malignant disease and head and neck involvement is relatively common. 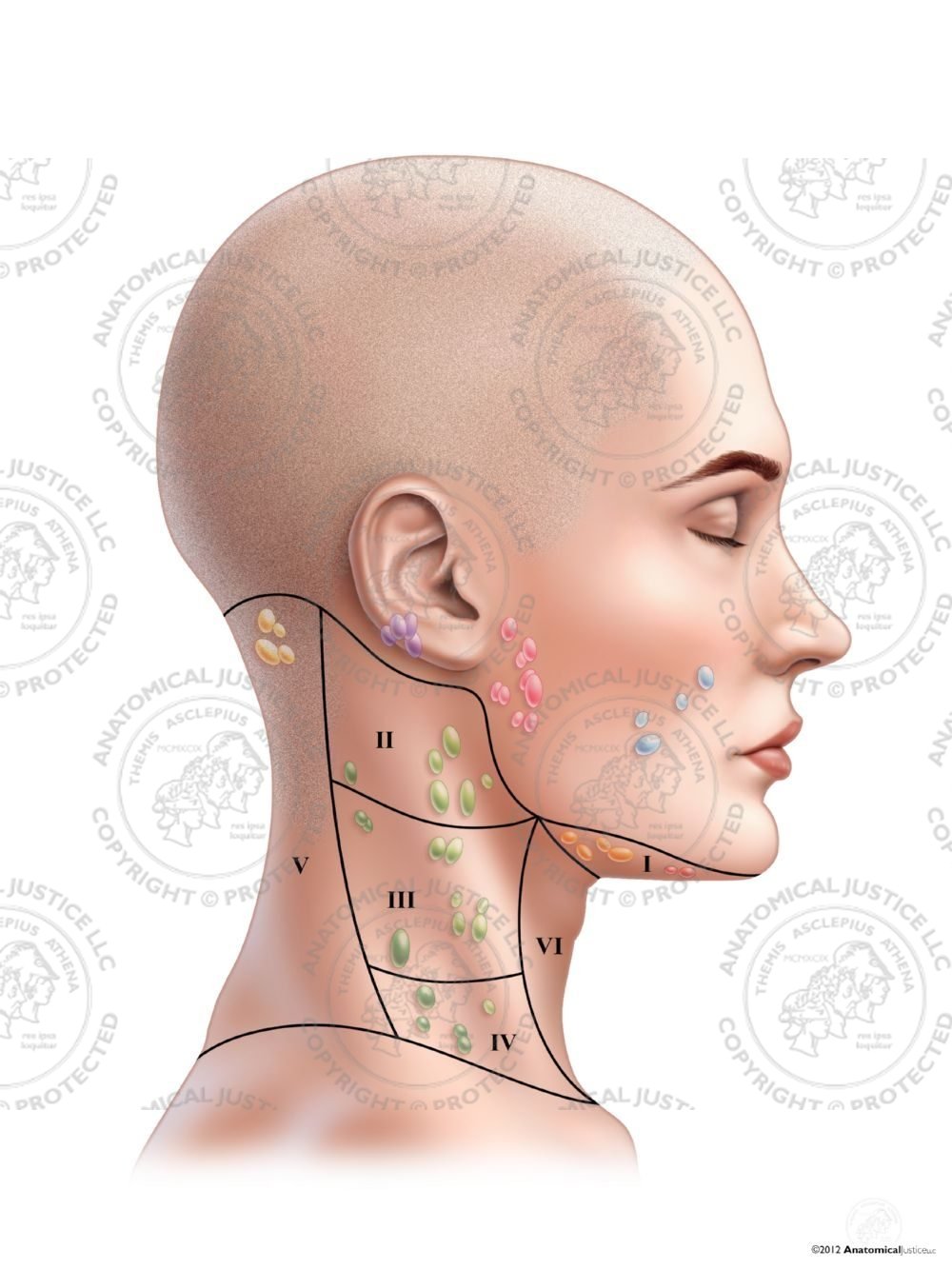
Moreover, metastatic nodes in an unexpected site indicates that the primary tumour is biologically more aggressive. Therefore, assessment of the distribution of metastatic nodes in patients with unknown primary may provide a clue to the site of the primary tumour. Metastatic cervical lymph nodes from head and neck carcinomas are usually site specific with respect to the location of the primary tumour. In patients with proven head and neck carcinomas, the presence of a unilateral metastatic node reduces the 5-year survival rate by 50%, whereas the presence of bilateral metastatic nodes reduces the 5-year survival rate to 25%. In addition, serial monitoring of nodal size and vascularity are useful features in the assessment of treatment response.Īssessment of nodal status is essential in patients with head and neck carcinomas as it predicts prognosis and helps in the selection of treatment options. Power Doppler sonography evaluates the vascular pattern of nodes and helps to identify the malignant nodes. Soft tissue oedema and nodal matting are additional grey scale features seen in tuberculous nodes or in nodes that have been previously irradiated. Grey scale sonographic features that help to identify metastatic and lymphomatous lymph nodes include size, shape and internal architecture (loss of hilar architecture, presence of intranodal necrosis and calcification). On ultrasound, grey scale sonography helps to evaluate nodal morphology, whilst power Doppler sonography is used to assess the vascular pattern. Neck nodes are also a common site of lymphomatous involvement and an accurate diagnosis is essential as its treatment differs from other causes of neck lymphadenopathy. Cervical nodal metastases are common in patients with head and neck cancers, and their assessment is important as it affects treatment planning and prognosis. Malignant lymph nodes in the neck include metastases and lymphoma. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
